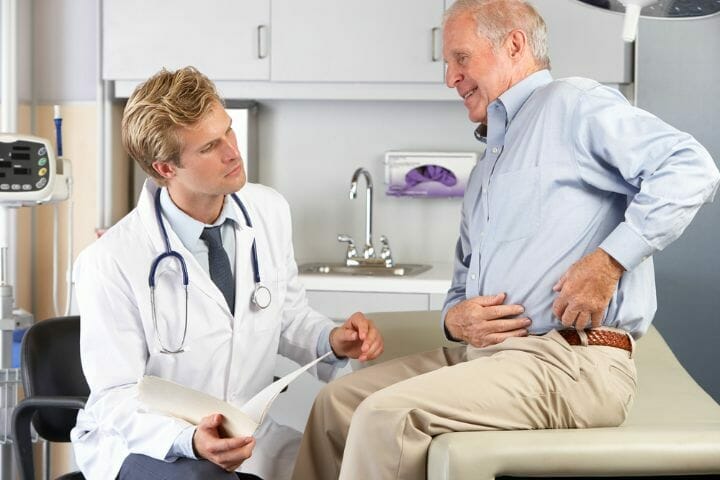
When can I sit on a normal chair after hip replacement? It depends on your physician’s restriction, pain on hips, and an approximate 6-8 weeks we will know. This leaves room for them to ask further questions on why is this necessary.
As physical therapists, we come in the picture upon referral, or even after the surgery itself. Mobility is already a concern from the surgeon, patient, and family as well.
Overall, being able to move and get out of the bed will be the first attempt towards function. Restrictions by the surgeon will be then evaluated, and fitted to what movement are not possible.
Contents
But What Is Hip Replacement Anyway?
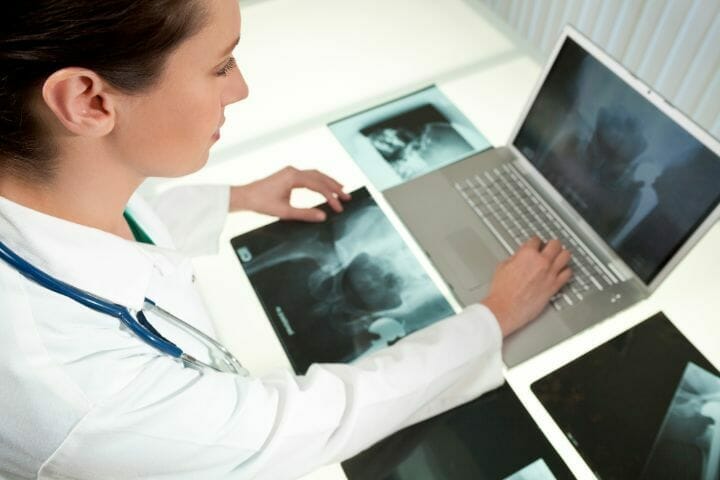
Most patients firsthand experience pain in their hips. Evaluation and assessment (MRI, CT Scan, X-ray) are acquired whether pharmacological (NSAIDS, paracetamols), and nonpharmacological management (physical therapy, mobility regimes, and rest) will relieve it. But if the damage/fracture has these following features, surgery is an absolute option:
- Unbearable weight-bearing of the leg (unable to stand or walk with it)
- Fractures that appear shattered (comminuted) or displaced.
- Severe arthritis causing abnormal growth of bone on the area
- Injuries that damaged the blood flow on the area, causing necrosis leading to death on the area
- Displacement and mobilization techniques are not permitted
- Congenital in nature, which needs replacement every few years as the child grows
According to the John Hopkins Medicine, hip replacement is operation to replace a worn-out or sore hip joint. The surgeon restores the old joint with an artificial joint. The artificial joint is a permanent replacement to either a damaged, fractured, or old joint due to arthritis.
There are three types of hip replacement: total hip, partial and hip resurfacing. Total hip replacement is the most common type, and replacement from both sides of the femoral head joint is necessary. But if the injury is partial, one side of the femoral head is the target. Hip resurfacing on the other hand is the replacement of the socket.
You may also like Best Hip Protectors for Seniors
Prevalence and Common Conditions of Hip Replacement
The prevalence of total hip replacement at fifty years of age was 0.58% and increased to 1.49% at sixty years, 3.25% at seventy years, 5.26% at eighty years, and 5.87% at ninety years of age. This means, that most of the elderly population as they grow older opt for the said operation due to frailty, disabilities from arthritis, and falls.
From Arthritis Health, about 90% of people who undergo hip replacement have osteoarthritis. It is a common condition that causes hip replacement due to degeneration in the area. Or decrease the ability to endure weight-bearing from muscles involved in the area, displacing or weakening the attachment of the hip bone.
Other conditions that are considered for surgery:
- Osteonecrosis – or avascular necrosis (AVN) is a condition wherein the nutrition on the area of the bone has decreased or diminished. AVN of the head of the femur forms one of the major indications for total hip replacement. Between 5-12% of the total hip replacements are performed in patients who have AVN of the femoral head.
- Congenital displacement – hip dysplasia can have long-term effects on patients as we get older. Mainly when arthritis is severe, or for people older than 45-50 years. Hip dysplasia has unique features that need special techniques for hip replacement surgery to be as successful as possible.
- Traumatic Arthritis – it is caused by an injury, causing a wearing out of the joint. Over time, nonpharmacological management can be manageable. Surgery or total hip replacement will be the last resort when the joints are worn out. Young patients with post-traumatic arthritis of the hip have good long-term outcomes after THA.
- Bone tumors – it is rather an uncommon circumstance that patients with bone tumors in the area opt for surgery. Usually, the tumor itself has grown on the hip bone. Removal of the tumor may include it, therefore hip replacements are needed.
Steps After Surgery
After surgery, management of pain medication by the mouth of IV will be administered. The development of blood flow clots may occur within the first few hours of immobility. Compression boots (devices that are worn around the legs and that inflate periodically) are often worn to prevent blood clots. Compression stockings may also be recommended.
After that, physical therapy comes into play for the recovery process of the patient. It may only depend on what procedure were you given. Guaranteed precautions will be at play once it is determined. A total hip replacement, with the most common procedure, posterior surgery will not be permitted to do abduction >30 degrees, external rotation and internal rotation of the hip.
Most motions on the affected area will be limited. With the only amount of range possible, careful and proper instructions on doing movements on the bed are done. Limited flexion, extension, and abduction will be done. Ankle pumping is instructed for active motion and preventing edema. Proper position on the bed will also be done.
Once you’re instructed on mobility on the bed, you’ll be instructed to get up on the bed and walk for short distances at the hospital. This will include the use of an assistive device that is appropriate for your condition. A walker or crutches will be provided, depending on the surgical procedure and expected recovery. Younger patients recover faster and use one crutch.
Motions That Are Not Allowed For The First Weeks After Hip Replacement
- Sleeping while lying down on the back without any proper support on the neck, trunk, and pillow between each leg. This will prevent the crossing of your legs whenever you are sleeping.
- Sleeping on the affected leg. If you want to side lie, you can sleep facing the unaffected leg’s side. Still with a pillow between each leg, to prevent a crossing of the legs and displacement. This can be eased, as pain is relieved in the area. Or the motion is particularly tolerated over time.
- Crossing your legs. Procedures that include the posterior area as the main surgical produce are not advisable to cross their legs. Adduction is a motion of the leg to draw it inwards. Displacement can occur, and surgery will be needed.
- Any bending activities that include wearing shoes, reaching toes, or picking up on an object are not allowed. It can cause displacement of the surgical prosthetic hip. Assisting the patient in wearing socks, lower extremity garments, or reaching anything lower than the trunk shall be provided. A long shoehorn could also be of help.
- Weight-bearing status shall be noted. Depending on the physician’s instruction, the weight-bearing status shall start from no weight at all, to partial. Patients may experience excruciating pain in doing it initially. Upon discharge, patients are expected to have a full-weight bearing on the affected leg.
You may also like Best Chair for Hip Replacement Patients
When Can I Sit On A Normal Chair After Hip Replacement?
Once you instructed to get up on the bed, you’ll be given a few minutes to tolerate your position in sitting while preventing learning of the trunk. But motion on the operated leg will be limited and shall be in a straight position until pain decreases. You’ll also be placed in a wheelchair upon transport on your way home.
Concerns on sitting position are strengthening of the core, trunk, and arms. Your physical/occupational therapist to be able to provide proper position precautions, and training for the first few weeks.
Guidelines
- Preventing sitting for more than 90 degrees, or if sitting in a chair, make sure that you don’t exceed the desired angle permitted. In addition, don’t let your knees raised higher than your hips. It can cause complications of impingement, interruption of blood flow, or displacement.
- Sitting on soft sofas. A firm cushion is possible to be sat on whenever you need to sit on a sofa. A recliner can be an alternative for you to sit on, but make sure that it’s firm and not broken (recliners that recline without any controls).
- If possible, have a chair commode beside the patient’s chair or bed to make bowel and bladder movement easier for the patient. Over time, training on the toilet can be initiated. Therefore, toilet seats need to have toilet risers and handles if possible. You can check wheelchairs with chair commodes here. Also, bedsides commodes to purchase at home.
- To sit down, have the chair on your back and the walker in front of you. Then hold on to the chair handle for support. With the operated leg maintained in a straight knee position, use the unoperated leg to fold and lower yourself to the seat. As slowly as possible, and make sure that you’ll be sitting in a firm chair to prevent bending of hips.
- When you get into a car, back up to the seat of the car, and then sit and slide across the seat toward the middle of the car with your knees about 12 inches apart. A plastic bag on the seat can help you slide in and out of the car easier.
Lastly, patients with a hip replacement, of whatever kind, will only be able to tolerate sitting positions as the pain has reduced. Moreover, updating your physician frequently about your weight-bearing status and precautions after 4-6 weeks are the only way to know if you can sit in a normal chair.