Do you find yourself unable to enjoy meals because of digestive distress? This guide will help you diagnose and combat common digestive problems in elderly.
Contents
Research shows more than 70 percent of the human body’s immune response lies in the digestive system as it actively works to break down foods, regulate hormones and neutralize toxins. Every organ system relies on the digestive system to receive its share of nutrients for survival.
Additionally, the gastrointestinal or digestive tract is often called the second brain by researchers and scientists because it is responsible for producing and releasing vital neurotransmitters that maintain our cognitive health. With age, the stomach starts to produce less acid, which plays a crucial role in regulating digestion.

This means that poor digestive health among older adults can cause symptoms that keep them in the bathroom longer but also make them more vulnerable to infectious diseases, autoimmune disorders, and trigger depression/behavioral anomalies.
As you grow older, you might notice yourself suffering from a “bad stomach” often. This distress can be attributed to a slowing down of the digestive system. Thus, we bring you this guide to help you understand what is bothering your digestive system and the steps you can take to improve its functioning and your overall well-being.
The Digestive Diseases
Constipation
Symptoms:
- Painful bowel movements
- Extremely infrequent bowel movements – less than three times in a week
- Hard stool consistency
The large intestine fails to operate with as much agility as it did in youth; it takes a while for the food waste to pass through the colon resulting in increased water absorption and reduced muscle contractions.
Seniors with Parkinson’s disease also commonly complain of constipation as disturbances in the nervous system negatively impact the intestinal tract.
Naturally, we can observe a higher prevalence of chronic constipation in the elderly. Older adults are also more likely to engage in zero to minimum physical activity throughout the day due to physical disability, which aggravates their constipation.
Diverticular disease
By the age of 50, almost one-third of the American population suffers from a type of Diverticulosis disease. Here, small pockets or diverticula form in the colon lining, which tends to protrude along the intestinal wall due to inflammation.
This inflammation can be brought about by :
- Medicine like NSAIDs
- Obesity
- Smoking
While some people do not experience any noticeable symptoms, others go through intense chills, vomiting, constipation, and cramps on the lower side of the abdomen when the pockets tear or explode.
Diverticulosis doesn’t have a specific treatment except for symptom management through painkillers and antibiotics. However, adopting a liquid diet can prove to be very helpful in easing your stomach and healing your diverticulosis as they require your digestive system to work less.
Under a liquid diet, you can eat soup, juices, milkshakes, frozen yogurt, and pudding. Avoid going overboard on the fiber content all at once since your stomach will be more sensitive during this time.

Gastroesophageal reflux disease (GERD)
The strength of contractions and tension in the upper esophagus considerably decreases with the natural aging process. As a result, Gastroesophageal reflux disease (GERD) has emerged as the most common GI condition among the elderly.
In GERD, the stomach acid wrongly refluxes into the esophagus to cause symptoms like :
- severe heartburn
- Sore throat and cough
- Chest pain
- Difficulty in swallowing
- Nausea
- regurgitation
If persistent GERD symptoms are left undiagnosed and untreated, the senior may have esophageal cancer in the future. GERD can also contribute to causing other GI complications like Barrett’s esophagus, esophagitis, and strictures in the esophagus.
However, acid reflux is also caused by older adults eating unhealthy fast foods that their bodies cannot digest, leading to spurts of weight gain and obesity.
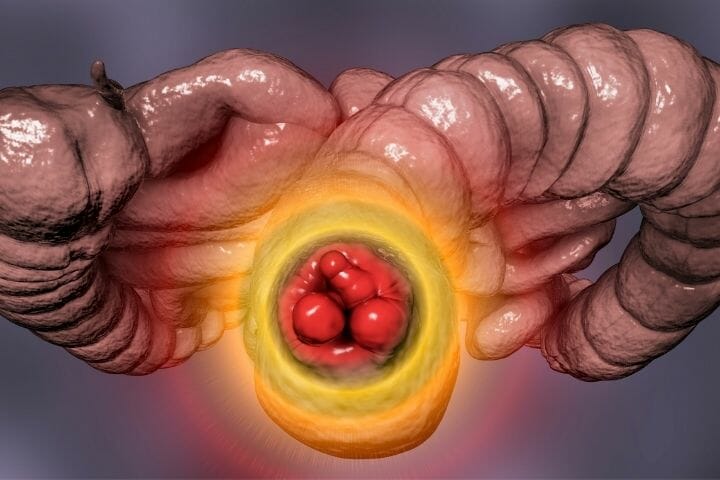
Colon cancer
After the age of 50, the tendency of the body to produce small growths known as polyps in the colon increases. These growths can be completely non-malignant but may also turn into colon cancer over time.
As per the American Cancer Society, colon cancer is the second leading cause of cancer death in America. Aged individuals with Crohn’s disease of the colon and ulcerative colitis or those who have immediate family members diagnosed with colon cancer are at the highest risk of getting diagnosed with the same themselves.
Therefore it is recommended for the elderly, especially men, to get routinely screened for colon cancer by a colonoscopy or a fecal immunochemical test (FIT). Only a colonoscopy can facilitate identifying and removing the polyps before it’s too late.
The earlier the cancer is detected, the more effective its treatment can be.
Hemorrhoids
The weakening of muscles around the esophageal sphincter leads to the formation of hemorrhoids – swollen veins around the entrance of the lower gastrointestinal tract.
Hemorrhoids are commonly found among the elderly, as they suffer from chronic constipation. Difficulty in your regular bowel movements strains the veins in the rectum area and makes them larger. This condition is characterized by itchiness and irritation.
Non-alcoholic fatty liver disease
The elderly who have diabetes or high triglycerides in their blood are susceptible to developing the non-alcoholic fatty liver disease – which causes inflammation in the abdomen and scars the liver tissues.
Irritable Bowel Syndrome (IBS)
IBS is among the common digestive disorders that the elderly suffer from; it is characterized by symptoms such as back pain, fatigue, constipation, and bloating.
Causes of the Digestive Problems
Inactivity
Nearly 10% (19mn) older adults face some form of mobility issues. This is one of the primary causes of constipation. Several older adults undergo knee or joint-replacement surgeries or suffer from diseases, which keep them on bed rest on a temporary basis and prevent them from moving around.
Dehydration
Staying hydrated becomes a challenge for the elderly who take diuretics to manage their chronic heart conditions. These medicines lower your blood pressure by making you lose water through excessive urination. Seniors are also at a higher risk for dehydration because their sense of thirst deteriorates over time. Some older adults might forget to drink water because of cognitive disabilities like Alzheimer’s disease and dementia.
Medication
In America, an adult over the age of 65 will be taking an average of five pills every day. Older adults are on the use of several drugs for their diverse illnesses and health conditions. Unfortunately, a cure to one disease can also cause another disease. Calcium chain blockers are used to manage high blood pressure and can induce constipation.
Commonly prescribed antidiabetic medicines like Metformin can also have lasting effects on the gut by causing diarrhea, dyspepsia, and vomiting.
Drugs like methotrexate and Imuran, which aim to treat rheumatoid arthritis and cancer in its early stages, damage the important parts of the small intestine to cause bloating and malnutrition.

Neuroleptic medication used to remedy Alzheimer’s disease and depression among seniors leads to colon degeneration.
Proton pump inhibitors are associated with the risk of small intestinal bacterial overgrowth (SIBO). The main symptoms of SIBO are nausea, bloating, and gas.
Geriatric patients are among the highest consumers of nonsteroidal anti-inflammatories NSAIDs to deal with their osteoarthritis pain.
NSAIDs like aspirin and ibuprofen are potentially dangerous as they erode the stomach lining that protects the stomach from the acid present to aid in digestion. They put the senior at a higher risk of developing severe gastritis and mucosal injury in the GI tract, with symptoms like :
- Heartburn
- Internal stomach bleeding
- Nausea
- Abdominal Pain
- Diarrhea
- Ulcer
Always take your NSAIDs along with heavy metals, and never consume more than the prescribed dosage. In addition to that, closely monitor your gastric symptoms, stool color and inform your doctor at the sight of any blood.
Gravity
The diaphragm is likely to sink after a certain age, causing the barrier between the esophagus and stomach to become less reliable and result in a hiatal hernia. Naturally, this hernia allows the stomach acid to reflux quickly, causing heartburn and GERD.
Hormone Changes
This is because these ovarian hormones regulate the intestinal muscles. The hormonal changes explain the worsening of IBS and GERD symptoms among women when they are on their periods.
On the other hand, women complained of constipation and increased abdominal fat after their menopause because low levels of estrogen cause constipation.
Steps to Take to Better Your Digestive Health
Watch Your Weight
Maintaining a healthy weight is beneficial for your digestive issues and your overall health. You might find yourself gaining weight more quickly now that you aren’t as physically active due to health restraints, but it’s important to keep a watch on your portion sizes and have small frequent meals to avoid overeating and indigestion.
Practice mindful eating by turning off the TV and smartphone and paying full attention to your food and its aspects. We often forget that digestion starts in the mouth; mindfulness can improve your chewing and help alleviate several digestive symptoms like gas and heartburn.
Since it can take over 20 minutes for your brain to realize when your stomach is full, you must slow down to notice your fullness and hunger cues.
A healthy diet
Eating a balanced diet filled with essential proteins, vitamins, minerals, and healthy fats is the first step towards ensuring good digestion. You must increase your intakes of foods like flaxseeds, chia seeds, walnuts, and fish high in omega-3 fatty acids to prevent inflammatory bowel diseases.
Fiber
It is no secret that fiber plays a vital role in better nutrient absorption and bowel health. A high-fiber diet has been proven to control the symptoms of digestive diseases like diverticulitis, reflux, and hemorrhoids.
While soluble fiber softens and bulks up the stool by absorbing water, insoluble fiber aids to keep everything moving in the digestive system.
Here are foods that are good sources of fiber :
- Raw fruits and vegetables
- Legumes
- Whole Grains
- Nuts and Seeds
The elderly should eat a minimum of five servings of fruit and vegetables to get their antioxidants.

Avoid triggering foods
As you age, you should stay away from processed foods, red meat, and refined carbs like white bread, pasta, rice, and other baked goods.
The trans-fats found in most processed foods are linked to a high risk of ulcerative colitis and bowel cancer. Studies have also found that consuming ice-creams and low-calorie drinks containing artificial sweeteners cause bloating and diarrhea in more than sixty percent of older adults.
Get tested for food allergies and sensitivities to help identify foods that trigger stomach issues and heartburn. For some older adults, gluten can lead to bloating, while in others, dairy consumption can cause diarrhea due to lactose intolerance.
Consider supplements
Probiotics refer to the good bacteria that can enable the elderly to achieve optimal digestive health by helping the body fight off infections. They are commonly found in yogurts and fermented foods/drinks such as kimchi, kombucha, and sauerkraut.
Probiotic supplements effectively get rid of Vitamin B12 deficiencies and other digestive issues like constipation and abdominal pain. Glutamine and zinc supplements also can provide supportive care to your leaky gut.
Hydration
Make sure that you stay hydrated by drinking eight to ten glasses of water per day. If you live in a tropical and humid climate, you might need more fluids. In addition to water, you can drink beverages like seltzer water, coconut water, fresh juice, and herbal teas to meet your fluid intake goals.
Even including vegetables and fruits with a high water content like cucumber, tomatoes, watermelons, and peaches in the diet can help to ease constipation.
However, you must strictly cut down on alcohol and caffeinated drinks like coffee and tea since they can severely dehydrate you.

Check your medications
As we have discussed before, several medicines can negatively impact your digestive system. It is imperative to inform your doctor about all the side effects you are experiencing and ask for an alternative if the medicine interferes with your quality of life.
Exercise
Getting regular moderate physical activity can prove highly beneficial for your digestion-related issues. Aim to exercise for at least 20 minutes every day to increase the frequency of your bowel movements and prevent constipation.
- Walking – Brisk walking can help stimulate the digestive system into movement, enabling a smooth passage of the food.
- Biking – You must add cycling to your cardiovascular fitness routine since it can help keep constipation at bay by decreasing the water loss in your stool. Also, biking is an effective way to reduce belly fat, which in turn will ensure higher efficiency in digestive functions, less bloating, and increased energy levels.
- If you want to keep your abdomen muscles active and prevent gas, exercises such as crunches and sit-ups are your one-stop answer.
- It is recommended to complete the core workout on an empty stomach instead of after meals. Start with ten sit-ups initially and then advance as much as you feel comfortable, depending on your existing health conditions.
- Having health conditions like diabetes, Parkinson’s disease and sclerosis weakens the pelvic floor muscles of the elderly and causes fecal incontinence. Squeezing and relaxing the pelvic floor muscles can play a vital role in dealing with overactive bladder and bowel control issues. Start by incorporating 25 to 50 repetitions into your workout routine.
Yoga
Diseases like Irritable Bowel Syndrome are triggered mainly by excess stress. Yoga can assist the senior in creating a better mind-body balance and getting rid of stress in life. Yoga poses that can help in achieving optimal digestion include:
- Downward dog and Upward Dog
- Triangle
- Boat
- Thunderbolt Pose
- Child’s Pose
- Reclining butterfly pose
Practicing these yoga poses consistently will relax the abdomen muscles, alleviate the symptoms caused by digestive conditions and build the senior’s core strength.

Maintaining Oral Health
Dental decay can cause an exacerbation in your digestive symptoms because the decayed teeth can only handle soft and mushy foods which are completely lacking in fiber. Good oral health can also help you ward off digestive issues.
Go for routine dental checkups and brush, floss your teeth daily to ensure that your teeth stay healthy. Alongside, the elderly also experience a decline in their saliva production which significantly affects the digestive system.
Stress
Dealing with excess stress can increase gastric acid production, which causes indigestion and reflux. Even though stress doesn’t directly lead to any digestive diseases, it can flare up your existing digestive conditions. Thus, please take care of your mental health, participate in activities that release endorphins, and get enough sleep.
Wrap Up
Now, you know that the digestive system of older adults reacts differently after being influenced by the body’s natural aging process. Only efforts to bring about simple lifestyle and dietary changes can take you a long way in leading a happy and healthy life, free from any digestive discomforts.

However, if you persistently experience symptoms such as bloating, constipation, diarrhea even after adopting lifestyle changes, you must book a consultation with your primary doctor and get your digestive organs screened to rule out the possibility of any serious underlying cause.
If this guide has helped you navigate your journey to good digestive health, please spread the word within your friend/family circles and on your social media profiles. Please drop a comment below with your potential queries or suggestions that can help improve this article.
We will try to get back to your queries as soon as possible and add any mistakes that we have made to the article to make it more complete.
