Living with diabetes isn’t just about watching your sugar levels and testing your blood glucose, there are other side effects of having diabetes that those living with this condition will need to watch out for.
One of the biggest side effects, when diabetics do not take care of themselves very well, is issues with their legs and feet. Medicare does provide benefit coverage for diabetics – their insulin and needles, for example – but many people with Medicare may not be sure if there is coverage for auxiliary issues, like foot care.
Medicare And Foot Care
When it comes to foot care, Medicare divides these services into two categories; treatment for serious conditions the health of your feet or your overall feet, and every day concerns like calluses.
Medicare will only provide coverage for treatments that are considered medically necessary for your health or to prevent serious future health concerns.
For the most part, Medicare will not pay for regular, routine foot care that is not related to a serious, ongoing medical condition. If you have Medicare Advantage, though, you may have access to additional coverage the those with just regular Medicare don’t have.
You might like to read: Is Diabetes a Disability?
Types Of Footcare Medicare Covers
As mentioned, Medicare will cover medically necessary foot care services that are to help with prevent the worsening of an ongoing serious medical condition, or stop it from getting any worse.
Before any services can be covered by Medicare, they will first need to be prescribed by a doctor or other medical professional. Additionally, the services will need to be performed by qualified podiatrist but sometimes they will cover it if it’s provided by another qualified physician – which will be evaluated on a case by case basis.
The services for footcare will be covered under your Part B benefits, and it generally includes treatment for
- Wounds
- Infected nails
- Injuries
- Heel spurs
- Hammer toes
If the foot care is administered while you’ve been admitted to a hospital then it will be covered under your Part A benefits although it still must be considered medically necessary in order for it to be totally covered.
Does Medicare Part C Offer More Footcare Coverage?
If you have Medicare Part C, or Medicare Advantage, then you may qualify for more benefits regarding foot care.
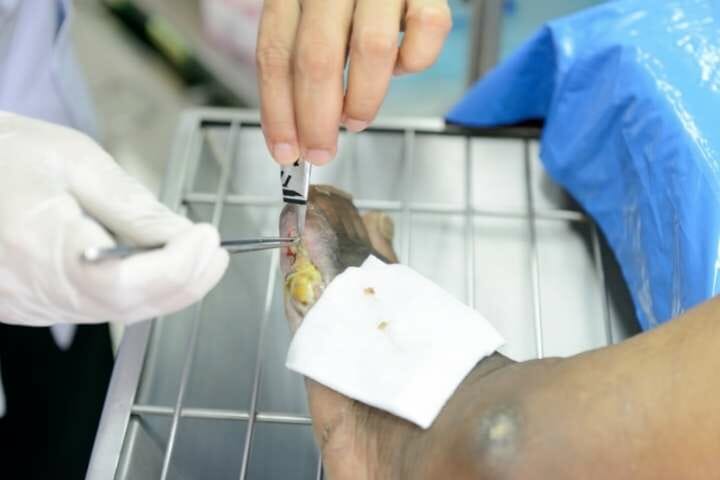
These plans may even include routine foot care in their covered benefits, but you will have to check with your plan for specific coverage details. You should check for coverage before booking any appointments as you may need to ensure you choose an in-network provider for the care appointment.
You might like to read: Insulin Pumps for Diabetes Patient
Why Is Diabetic Footcare Medically Necessary?
Those who have diabetes have an increased risk of serious foot problems, especially if they do not take proper care of themselves and look after their condition.
With diabetics, many of their leg and foot issues stem from something called neuropathy, which is nerve damage to the area. Over time, with prolonged damage, it can make it so that you don’t have feeling or sensations in your feet. This can make it especially difficult to know if you have somehow injured your foot or have an open wound.
Diabetics are also especially vulnerable to ulcers and damage to the skin, and those things can become infected. If there isn’t any sensation in a diabetic’s foot then they may not know if there is an infection present.
Further, having diabetes can mean that the blood flow to your extremities can be affected, This additional factor can lead to serious infections that could, if not treated properly, lead to an amputation.
This combination of reasons is why Medicare considers foot care medically necessary for those who have diabetes.
Which services and equipment are covered for those with diabetes?
When it comes to medically necessary foot care for those with diabetes, Medicare will cover regular nail trims, callus and corn removal as well as special shoes and inserts.
In order to get these services covered by Medicare, you will need an official diagnosis of diabetic neuropathy from your doctor. After this diagnosis is on file with Medicare, you will then need to have an assessment done every 6 months after that to determine if your condition still warrants the footcare to be provided.
Additionally, if your podiatrist recommends it you can be covered by a single pair of extra-depth shoes or custom-molded shoes – including the fitting appointments to make sure they will work for your needs.
If you prefer inserts into regular shoes as opposed to having custom molded shoes, you may be able to get two pairs of inserts covered every year by Medicare or three pairs of extra depth inserts.
You might like to read: Cost Of Diabetes To Individual, Family, And Community
How Can You Qualify For Footcare Benefits With Medicare?
In order to get these benefits covered, you will need to be under treatment by a physician.
This healthcare provider will need to document that you have a medical condition that requires footcare to help prevent the worsening of this condition or that it is medically necessary for the person’s overall health.
Further, you will need to have been receiving active care for this condition for at least six months for Medicare to start paying for footcare benefits.
If you have a Medicare Advantage plan, you will need to make sure you use a provider that is in your plan’s network.
Will You Need To Pay Out Of Pocket For This Care?
Even if you have benefit coverage, you still may need to pay for some costs out of pocket when it comes to the footcare services.
Part B Benefits
Under this part of Medicare benefits, you will need to pay the same 20% like you would for any other service (provided you have already met your deductible amount). You will also need to make sure you have paid your Part B monthly premium – which is around $145 per month for most people.
Once this deductible amount has been paid, Medicare will pay for 80% of all the footcare services, equipment, diabetic footwear, and anything else considered medically necessary by your medical provider.
Medicare Advantage
If you are looking to submit any claims under your Medicare Advantage benefits for footcare, the coverage will vary depending on the plan you have and who the provider of that plan is.
There may also be different coinsurance costs, different deductibles and various monthly premiums. You may also need to make sure you choose an in-network provider to make sure the cost will be covered by your benefits.
You might like to read: Simple Steps to Lower Your Risk of Diabetes
Medigap
If you have a Medigap plan, you may be wondering if you can submit for footcare costs under this plan.
Unfortunately, at this time, Medigap plans do not provide any benefits for receiving foot care – even if it’s deemed to be medically necessary.
Even though Medigap doesn’t cover footcare services, this plan may pay for some of the coinsurance or any other out of pocket expenses you experience that your Part B coverage hasn’t paid for.
How Often Can You Receive This Service For Footcare?
If your doctor has determined that footcare is medically necessary for your condition, or to prevent your condition from getting worse, then you can receive this footcare benefit as often as you need it under your Part B benefits.
You will need to go in for an assessment every six months to make sure that your condition hasn’t changed and you still require the footcare benefits. Your doctor will need to submit this assessment to Medicare in order for them to continue covering the care.
It is also important to note that you need to be receiving footcare for at least six month prior to applying for coverage, and it will need to be the same footcare services that you are applying for benefit coverage now.
You might like to read: Can You Get Disability For Foot Problems?
In Summary
Getting footcare covered for conditions that affect your feet, like diabetes, is possible through Medicare.
You will need to see your doctor to get it documented that you have diabetic neuropathy and that receiving regular footcare will be beneficial to ensuring your condition does not cause your overall health to deteriorate.
If you are not sure about the current condition of your feet, and think you may need some wound care or callus removal, you can schedule an appointment with your doctor to determine what your best options may be.
Your doctor can document the condition of your feet, along with your diagnosis of diabetes, to recommend that you receive coverage for footcare.
You may still need to pay some out of pocket expenses (IE 20% under your Part B plan) but the majority of the care will be covered when you have a condition like this.
Regular footcare for people with diabetes can help prevent major infections from spreading and keep their overall health balanced, so spending the money now on providing that care can stop major costs in care down the road.
Make sure that your doctor documents all of your concerns with the condition of your feet so that there is a trail of issues and so that Medicare can see the history you have to determine what type of care they can approve you for.
